CHALLENGE
Our health system partner experienced an increase in Average Length of Stay (ALOS) in the acute setting and an increase in Skilled Nursing Facility (SNF) utilization. When we became their partner, our goals were to decrease acute length of stay for patients requiring post-acute care without an increase in re-hospitalization rates; increase Home Care utilization (goal of 22%); decrease SNF use (goal of 25%); and complement the hospitals ambulatory care initiative.
SOLUTION
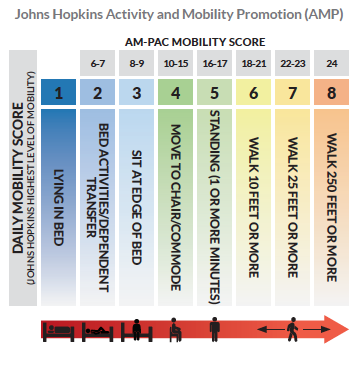
Collaboration was established between case management and PACCs at onset of admission, expediting the discharge process. During each shift, PACCs assess patient mobility based on the Johns Hopkins Tool. Identification of early ambulation and clearly outlined outcome parameters decreased reliance on therapy staff and reduced SNF utilization, as PACCs identified home care appropriateness sooner in the discharge planning process.
Patients received front-loaded/every other day visits for two weeks, which reduced re-hospitalization rates and supported an acute patient’s transition to home safely. Unlike most health systems, which rely on overburdened case managers and discharge planners tasked with long lists for home health referrals and follow-up, our team of community educators and clinicians are onsite at each partner hospital to facilitate home health referrals from day one. Our unique PACC program was designed to work inside a hospital, and touches every referral going to home health from day one. Being onsite allowed us to help providers manage post acute care systems rather than having patients on a list awaiting review for one to two days.
RESULT
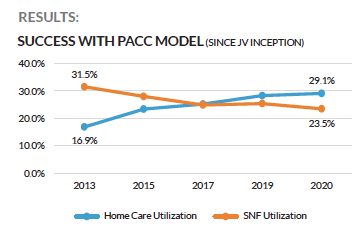
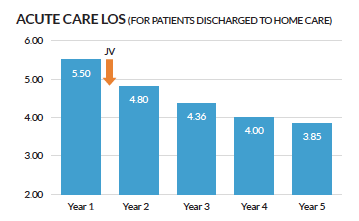
Between 2013 and 2020, the PACC Model increased home care utilization from 16.9% to 29.1%, and SNF Utilization dropped from 31.5% to 23.5%. Acute care length of stay for patients discharged to home dropped from 5.5 days to 3.85. Our value-based care partner also saw better margins by getting patients in home health sooner, with patients spending an average of 50 days in home health vs. 500 days in SNF.